The clinical literature on PRF can be confusing because multiple formulations exist, each prepared differently and suited to different applications. A patient told they will receive “PRF” during their procedure may receive L-PRF, i-PRF, A-PRF, or another variant — and the distinction matters clinically. This guide covers what each formulation is, how it differs from the others, and which situations each is most appropriate for. For the foundational PRF biology, see our PRF overview.
Why Centrifugation Protocol Determines PRF Type
All PRF variants start the same way: a blood sample is drawn from the patient and centrifuged to concentrate platelets, leukocytes, and fibrin in one layer. The centrifugation speed and duration determine what ends up in that concentrated layer and in what proportions. Higher speeds and longer times produce denser fibrin matrices with more structural integrity. Lower speeds produce softer, more gel-like or even liquid formulations. These physical properties map directly to clinical applications.
L-PRF (Leukocyte-Platelet Rich Fibrin)
Protocol: ~2700 rpm, 12 minutes. Produces a dense, resilient fibrin membrane.
Key properties: High leukocyte content, strong fibrin scaffold, sustained slow release of growth factors over 7–14 days.
Best indicated for: Bone grafting sites (mixed with particulate graft to bind it and add biological activation); extraction socket preservation; sinus lift augmentation; ridge augmentation; periodontal bone defect regeneration; wound coverage as a membrane.
i-PRF (Injectable PRF)
Protocol: ~700 rpm, 3 minutes. Produces a liquid to light gel rather than a solid membrane.
Key properties: Flowable and injectable; higher platelet count than L-PRF.
Best indicated for: Injection into periodontal pockets; mixing with bone graft materials to create a more mouldable, biologically active paste; sub-gingival injection for peri-implant soft tissue volume augmentation.
A-PRF (Advanced PRF)
Protocol: Slow centrifugation, longer duration. Produces a membrane with higher growth factor concentration than standard L-PRF.
Best indicated for: Gingival recession coverage (root coverage with connective tissue graft); periodontal plastic surgery procedures; anterior aesthetic cases where soft tissue quality and vascularisation of the graft are critical.
T-PRF (Titanium PRF)
Protocol: Standard centrifugation in titanium rather than glass tubes. The metal activates platelets through a different surface mechanism than silica glass.
Best indicated for: Implant sites where soft tissue integration around the implant neck is a specific goal; cases where membrane strength is a priority.
When Synthetic Materials Are Used Instead of PRF
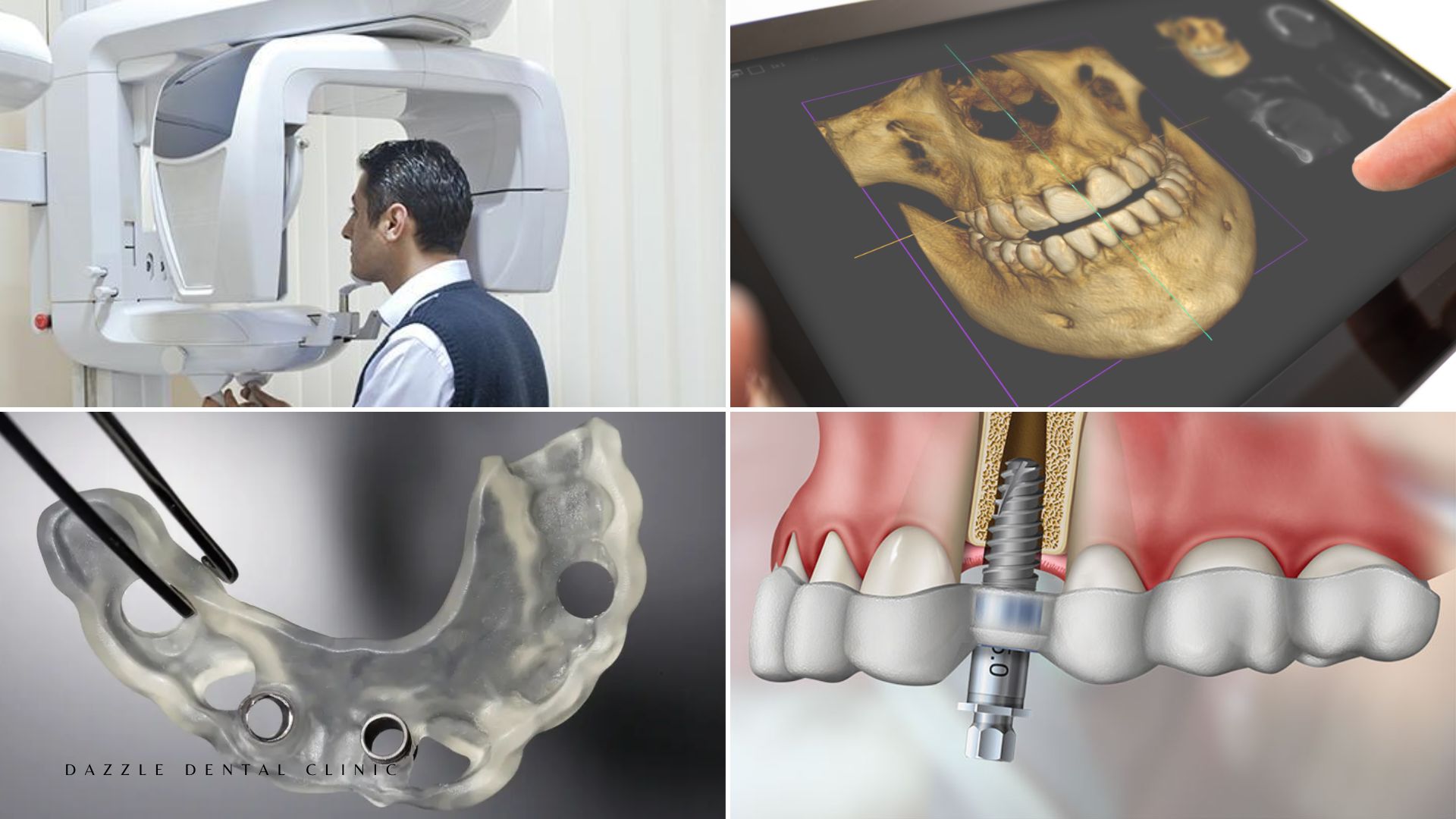
Mucograft (porcine collagen matrix), Alloderm (human acellular dermal matrix), Bio-Oss (bovine xenograft), and Bio-Gide (collagen membrane) are used when PRF alone is insufficient or when autologous tissue volume is inadequate. The combination Bio-Oss + PRF + Bio-Gide is the most commonly used protocol at Dazzle for horizontal and vertical bone augmentation.
FAQs
Q1: Can PRF be used in patients who have taken blood thinners?
This requires individual assessment. For minor antiplatelet use (aspirin), PRF is usually still viable. For patients on warfarin or NOACs, the clinical situation determines whether PRF preparation is appropriate. This is discussed at consultation for each patient individually.
Q2: Is PRF better than a bone graft alone?
The consistent finding across published studies is that PRF combined with bone graft produces better outcomes than bone graft alone: higher bone density at the graft site at 6 months, faster socket healing, better soft tissue closure. PRF does not replace bone graft material — it enhances the graft’s biological environment.
Q3: Does having PRF mean a longer appointment?
The blood draw and centrifugation add approximately 15–20 minutes to the preparation phase. In practice, this time is absorbed into the overall surgical preparation and does not extend the patient’s time in the chair by a significant amount.
Q4: Is there a difference in cost between PRF types?
The cost differences between formulations primarily reflect the consumable cost of the tubes and centrifuge protocol. The formulation selection is made on clinical grounds, not cost optimisation.

















.webp)