Platelet-Rich Fibrin (PRF) is a biological adjunct used at Dazzle Dental Clinic for specific surgical procedures where the clinical evidence supports meaningful benefit to healing. It is not a universal add-on to every treatment. Understanding what PRF does and when it is specifically indicated — rather than offered as a premium upgrade — helps patients engage more accurately with treatment recommendations that include it.
What PRF Is and How It Is Prepared
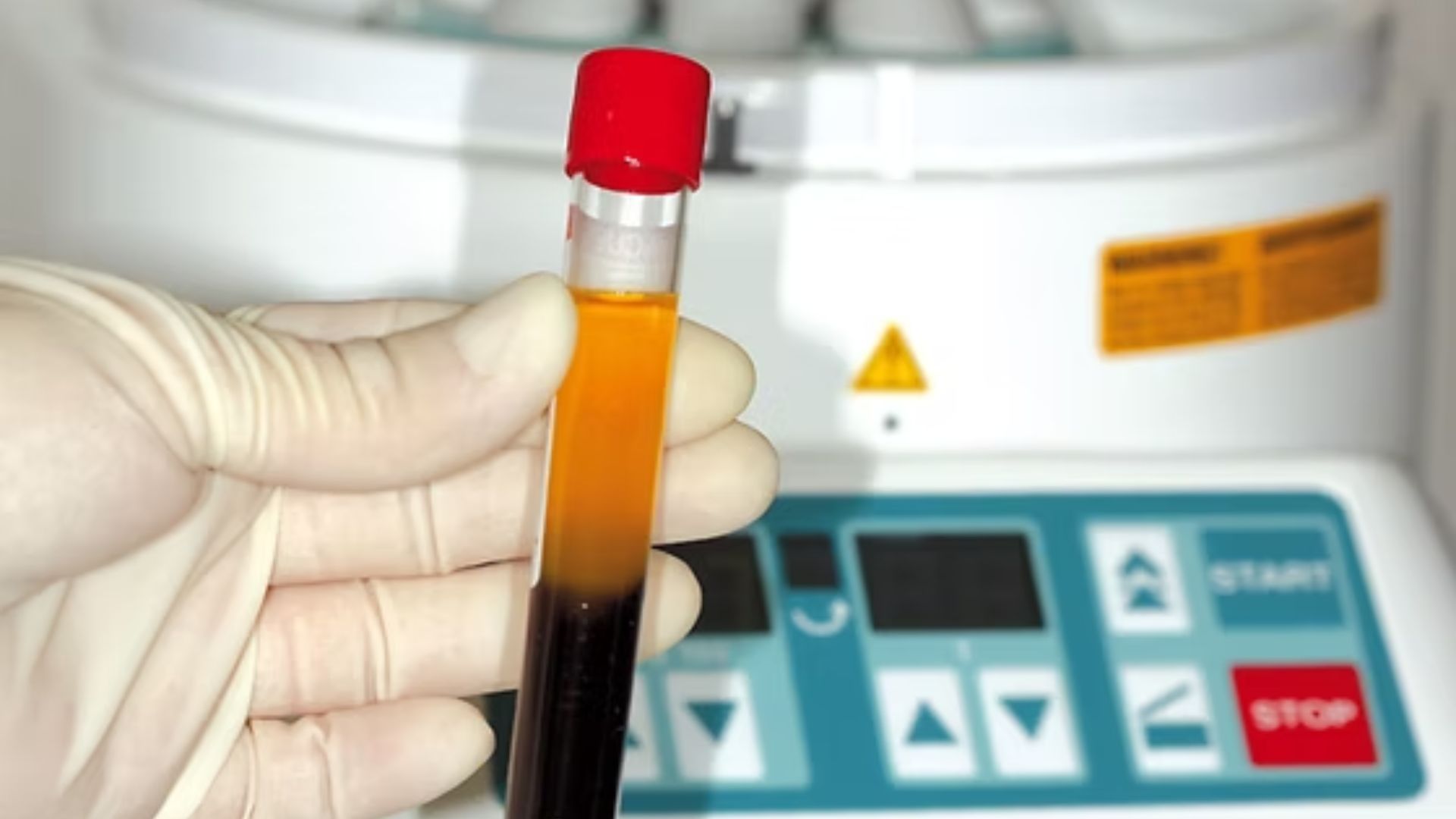
PRF is prepared from the patient's own blood. A small blood sample (20–40ml, from 2–4 standard tubes) is drawn at the clinic immediately before the surgical procedure and centrifuged for 10–15 minutes. The centrifugation separates blood layers: the middle layer is a fibrin clot concentrated with platelets, leukocytes (white blood cells), and the growth factors they contain. This clot — the PRF membrane — is placed at the surgical site.
Because it is entirely autologous, there are no rejection or allergic reaction risks. No anticoagulants, additives, or external biological materials are involved. For a full breakdown of different PRF formulations (L-PRF, i-PRF, A-PRF, T-PRF) and their specific applications, see our PRF applications guide.
The Three Growth Factors Responsible for PRF's Clinical Effect
PDGF (Platelet-Derived Growth Factor): stimulates osteoblast and fibroblast proliferation, driving new bone formation and angiogenesis. TGF-β (Transforming Growth Factor-beta): regulates cell differentiation, promotes collagen synthesis, and modulates the inflammatory response. VEGF (Vascular Endothelial Growth Factor): drives angiogenesis — the formation of new capillary networks that bring oxygen and nutrients to regenerating tissue. The fibrin matrix is also physically active: it supports tissue ingrowth as a scaffold and holds bone graft particles in position.
Where PRF Is Used at Dazzle
Bone grafting: The application with the strongest published evidence. PRF mixed with particulate bone graft consistently produces better bone density outcomes at 6 months than graft alone.
Sinus lift augmentation: L-PRF mixed with xenograft in the elevated sub-sinus space improves angiogenesis within the graft mass and shortens the healing period before implants can be placed by approximately 4–6 weeks in published series.
Tooth extraction sockets: L-PRF placed immediately after extraction maintains ridge volume, accelerates epithelial closure, and reduces post-extraction swelling and pain.
Implant placement in compromised bone: Applied at the implant site to support early osseointegration — most valuable in soft bone, complex socket anatomies, and patients with healing compromises such as controlled diabetes.
Gum surgery: Used alongside connective tissue grafts to improve graft vascularisation and accelerate healing in root coverage procedures and peri-implant tissue augmentation.
When PRF Is Not Added
Straightforward single implants in healthy, dense Misch Type I–II bone in medically uncomplicated patients may not benefit meaningfully from PRF adjunction. Routine extractions with no subsequent implant plan do not require PRF. At Dazzle, PRF is not added by default to every surgical procedure — the recommendation is made when the specific clinical indication is present.
FAQs
Q1: Is PRF safe?
Yes. Entirely autologous preparation from the patient's own blood: no allergy, rejection, or disease transmission risks. The centrifuge uses sterile closed-system tubes.
Q2: Does PRF extend the procedure time significantly?
The blood draw takes a few minutes; centrifugation 10–15 minutes. In practice, this time overlaps with anaesthetic preparation and surgical setup. Most patients do not notice a meaningful extension in chair time.
Q3: What is the difference between PRF and PRP?
PRP (Platelet-Rich Plasma) is an older formulation requiring anticoagulants — it contains chemical additives and releases growth factors rapidly in a single burst. PRF is additive-free and releases growth factors slowly over 7–14 days from the fibrin matrix — a more sustained biological effect. PRF has largely replaced PRP in modern regenerative dentistry protocols.
Q4: Is there an additional cost for PRF?
Where PRF is recommended, the cost is included in or itemised within the procedure fee. At Dazzle, the use of PRF is not a premium upgrade charged separately as an afterthought — it is planned as part of the surgical protocol and costed accordingly.

















.webp)