PRF is not a single product — it is a family of protocols that produce different fibrin preparations with different properties, suited to different clinical situations. Understanding which type is used for which application helps patients and referring clinicians evaluate treatment plans more specifically. This article covers the main PRF formulations and their distinct use cases. For the foundational biology of what PRF does and how growth factors work, see our PRF overview article.
L-PRF: The Foundation of Surgical PRF Use
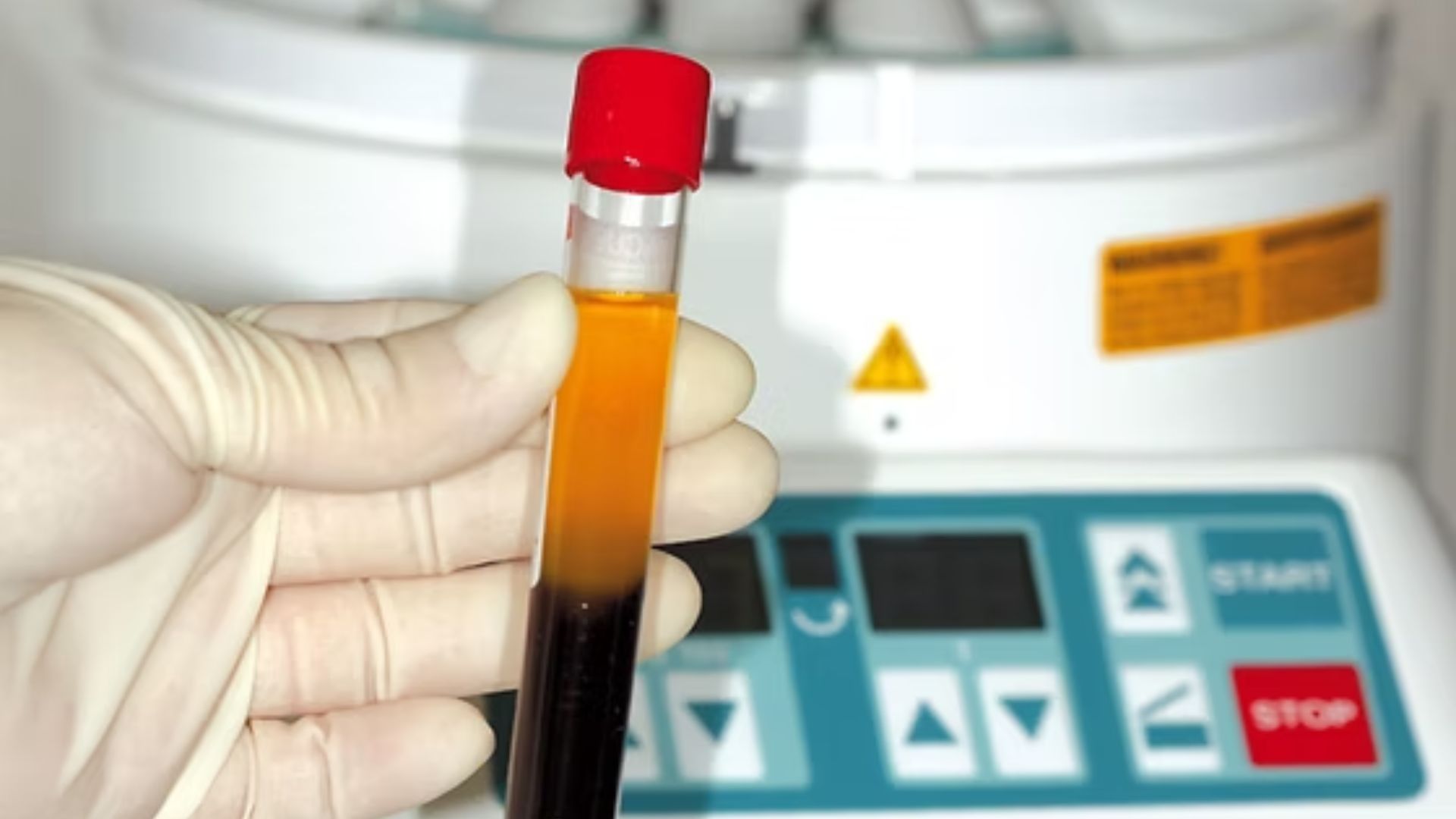
L-PRF (Leukocyte and Platelet-Rich Fibrin) is the most widely studied and most commonly used PRF formulation. Prepared by centrifuging blood at approximately 2700 rpm for 12 minutes, it produces a dense fibrin membrane containing a high concentration of platelets, leukocytes, and growth factors.
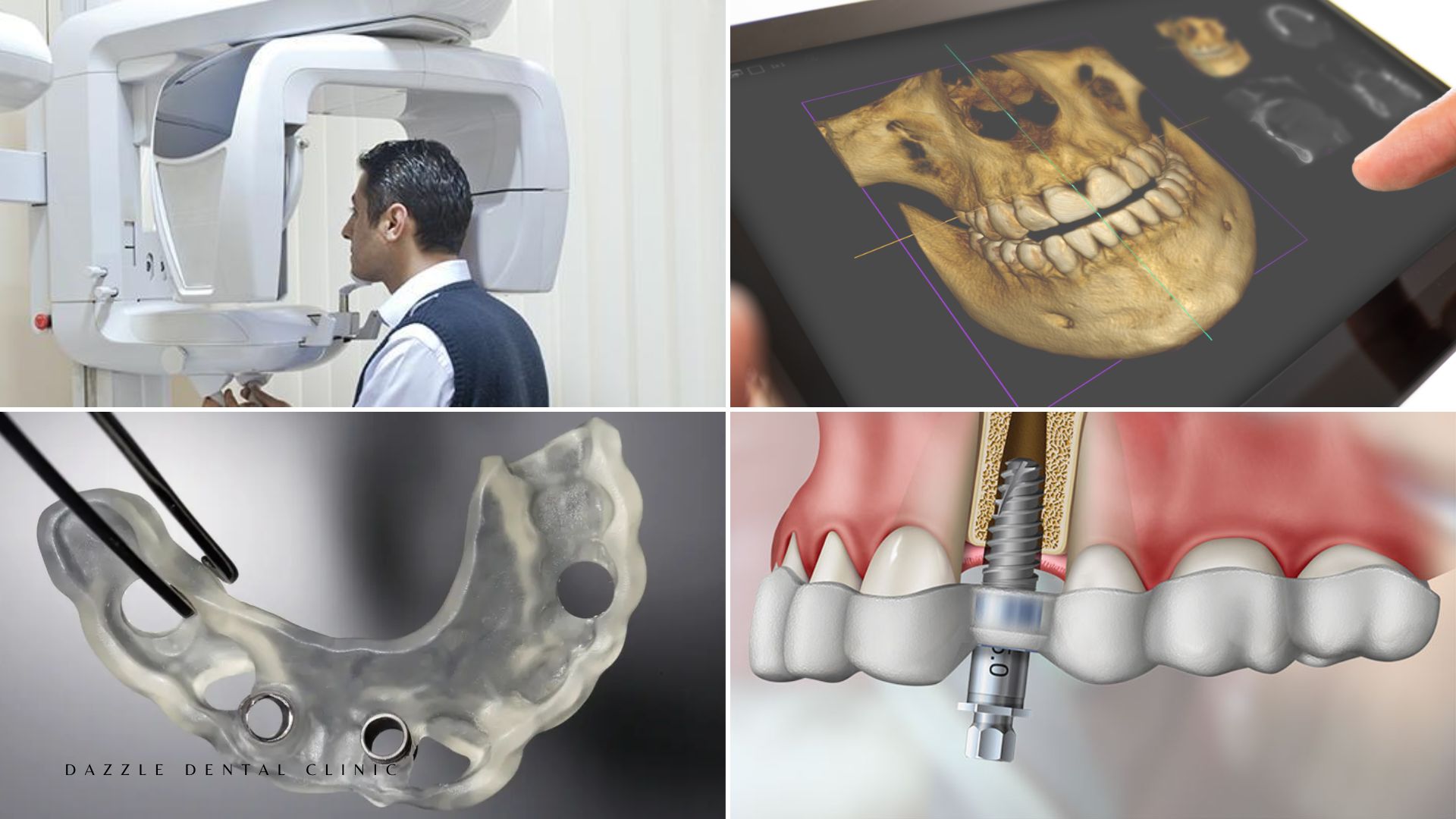
Primary applications: Intra-bony defect regeneration — L-PRF placed within bone defects from periodontal disease provides a scaffold and growth factor environment for bone regeneration; extraction socket preservation — placed in the socket immediately after extraction maintains volume and accelerates epithelial closure; sinus lift augmentation — L-PRF mixed with xenograft particles binds them in place, promotes angiogenesis, and accelerates new bone formation; horizontal bone augmentation — combined with bone graft material and covered with a collagen membrane. For a full overview of these guided tissue regeneration protocols at Dazzle, see our dedicated treatment page.
i-PRF: The Injectable Formulation
i-PRF (Injectable PRF) is produced at lower centrifugation speed, creating a liquid or gel-like formulation. Because it remains injectable, it can be mixed with other materials or delivered directly into tissue by syringe.
Best indicated for: Peri-implant soft tissue augmentation; periodontal pocket treatment; mixing with particulate bone graft to create a mouldable, biologically active paste.
A-PRF: Advanced Protocol for Periodontal Plastic Surgery
A-PRF (Advanced PRF) uses a slower centrifugation protocol to produce a fibrin matrix with a higher leukocyte and growth factor concentration, particularly well-suited for soft tissue procedures. Best indicated for gum augmentation and gingival recession coverage; periodontal plastic surgery cases where aesthetic tissue outcomes are critical.
T-PRF: Titanium-Based Preparation
T-PRF (Titanium PRF) is prepared in titanium rather than glass centrifuge tubes. Its primary application is in implant sites where enhanced soft tissue integration around the implant neck is a specific goal.
When Synthetic Materials Are Used Instead of PRF
Mucograft: A porcine collagen matrix for soft tissue volume augmentation and root coverage, used when autologous donor tissue is inadequate. Alloderm: Human acellular dermal matrix for gingival augmentation. Bio-Oss and Bio-Gide: The standard scaffold and membrane combination for guided bone regeneration. Combining Bio-Oss with PRF adds the osteogenic growth factor signal that makes the combination biologically more active than scaffold alone — the most commonly used protocol at Dazzle for horizontal and vertical bone augmentation.
FAQs
Q1: Which PRF type does Dazzle use most commonly?
L-PRF is the most commonly used formulation at Dazzle, covering the majority of implant, bone graft, and sinus lift applications. i-PRF is used for soft tissue injection applications. A-PRF is selected for periodontal plastic surgery cases where maximum growth factor concentration is indicated.
Q2: Do all patients having implants at Dazzle receive PRF?
No. PRF is applied where the clinical evidence supports meaningful benefit for that specific procedure. Bone grafting cases, sinus lifts, complex extraction sockets, and patients with healing compromises consistently benefit.
Q3: Is there a difference in healing time with PRF?
Published studies show meaningful differences primarily for bone graft sites — PRF combined with bone graft reduces the healing period before implant placement by 4–6 weeks in sinus lift cases in most published series.
Q4: What is the difference between Bio-Oss and the patient's own bone for grafting?
Autogenous bone (from the patient) is osteogenic — it contains living cells capable of forming new bone directly. Bio-Oss is osteoconductive — it provides a scaffold for bone to grow onto and through, but it does not itself form bone. The combination of PRF (osteogenic growth factors) with Bio-Oss (scaffold) approximates the biological environment of autogenous grafting with less surgical morbidity.

















.webp)