The shift from film to digital radiography in dental practice eliminated the darkroom, reduced processing time from 20 minutes to under 10 seconds, and reduced effective radiation dose by 70–80% compared to standard dental film. These are not incremental improvements — the practical impact on clinical workflow is significant. Diagnoses that previously required a separate appointment for film development now happen in the same appointment. Treatment can be planned and, for straightforward cases, begun in the same visit.
At Dazzle Dental Clinic, digital periapical radiography, digital panoramic imaging (OPG), and CBCT 3D scanning are the standard imaging modalities. All are available in-house with same-appointment delivery of results.
What Digital X-Rays Provide That Film Cannot
Digital sensors produce a higher dynamic range than film — they record a broader range of tissue densities in a single exposure, which reduces the number of retakes required for an adequate image. The image is adjustable: brightness, contrast, and zoom can be modified on-screen without changing the clinical information. This means the treating dentist sees the same raw data through different enhancement modes to extract the maximum diagnostic value.
For patients, this means: lower radiation dose (approximately 1–5 μSv per periapical image on digital vs 5–15 μSv on E-speed film); immediate review of the image with the clinician, rather than waiting for development; and digital storage with no degradation over time, easily transmitted to specialists or international patients’ home dentists.
The Clinical Role of Periapical Radiographs
Periapical radiographs (the small intraoral film-sensor X-rays placed beside the tooth) are the standard diagnostic tool for: periapical pathology (abscess, granuloma, cyst around root tips); root fracture assessment; interproximal caries detection; assessment of root canal treatment quality; implant marginal bone level monitoring; and crown or restoration margin fit assessment. At Dazzle, periapical radiographs are taken with a paralleling technique and film holder to ensure consistent image geometry — which matters when comparing images over time to track bone level changes at implants or periodontal sites. This feeds into the guided surgery and implant planning workflow.
OPG for Full-Arch Assessment
The digital OPG (orthopantomogram) provides a full-arch view of both jaws, all teeth, the sinus floors, and the inferior alveolar nerve canal in a single exposure (12–15 μSv on digital). It is used for: initial comprehensive assessment; third molar evaluation; general implant site screening before CBCT; orthodontic assessment of tooth positions and root development; and jaw lesion or cyst identification. The OPG is not sufficient alone for implant planning (bone width is not visible) but is the appropriate first-level screening tool before committing a patient to CBCT.
Real-Time Decision-Making in the Same Appointment
The practical value of same-appointment imaging is that the clinical decision does not have to wait. If a root canal is in progress and the working length file radiograph shows the file is 2mm short, the file is adjusted at the same visit. If a crown preparation radiograph shows the reduction is inadequate, it is corrected before the impression is taken. If a post-treatment periapical shows a missed canal or incomplete fill, it is identified while the patient is still in the chair. This immediacy reduces the number of appointments and improves clinical quality by eliminating the information lag that film processing created.
FAQs
Q1: How many X-rays will I need during a typical implant treatment?
For a single implant: a periapical or OPG at assessment, a CBCT for surgical planning, a post-placement periapical confirming depth and angulation, and periapical reviews at crown delivery, 6 months, and annually for the first two years. Total for a single implant: approximately 5–8 periapical or OPG exposures and one CBCT. The CBCT dose is typically the largest single exposure in this sequence.
Q2: Are dental X-rays safe?
Yes. A digital periapical X-ray delivers 1–5 μSv — less radiation than a single hour of flying at altitude (approximately 3 μSv/hr from cosmic radiation). The total dose from routine dental imaging over a year is negligible in terms of health risk. X-rays are taken at Dazzle only when the clinical information they provide changes the treatment decision — not as a routine at every appointment.
Q3: Can I request copies of my X-rays?
Yes. All images are stored digitally and can be exported in standard formats (JPEG for 2D images, DICOM for CBCT) and emailed to you, your home dentist, or a specialist. For international patients who have had imaging done at Dazzle, this is provided as a standard part of the discharge documentation.
Q4: What is the difference between a periapical X-ray, an OPG, and a CBCT — and when is each used?
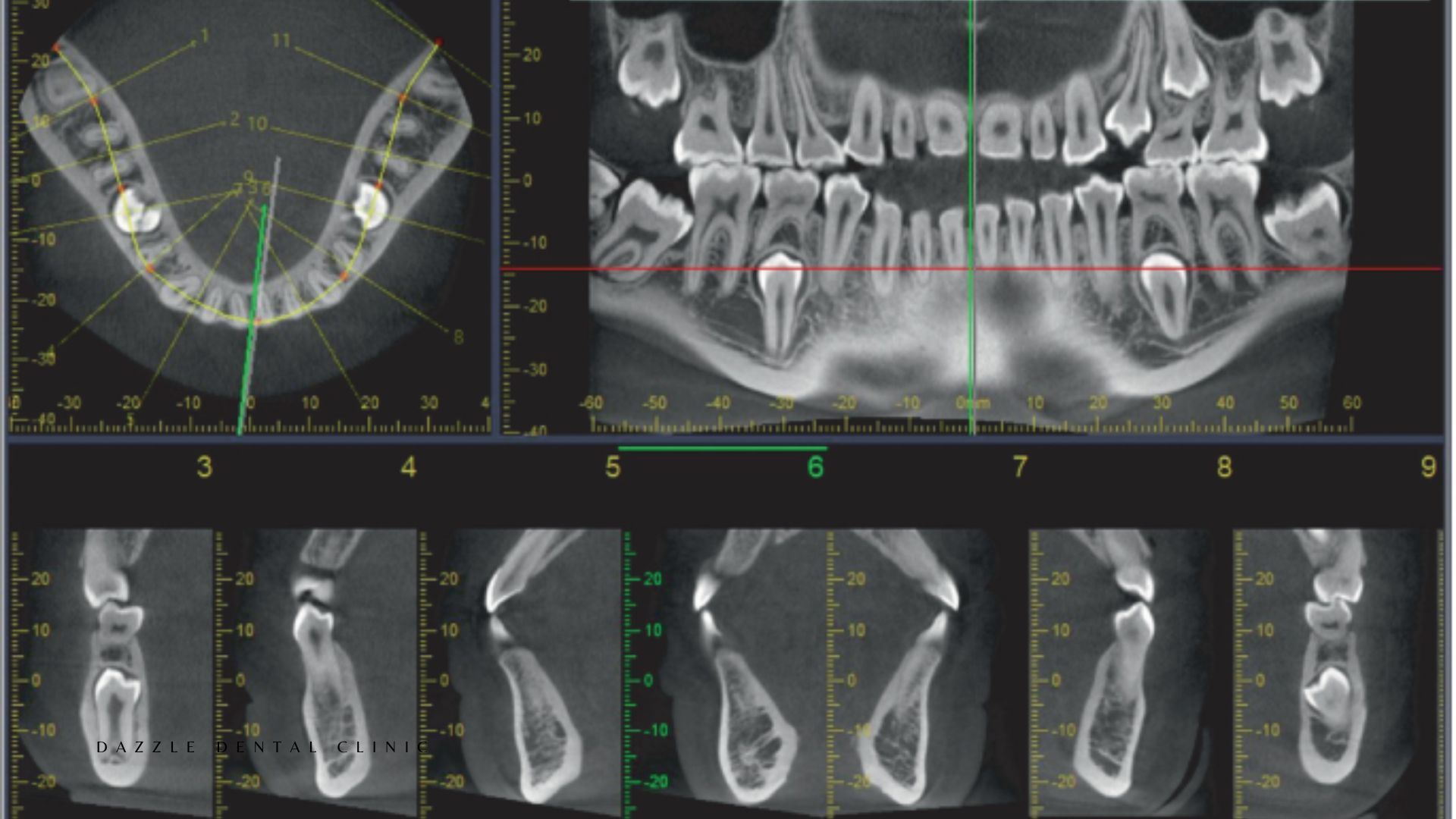
A periapical shows 2–3 teeth in detail; used for diagnosis of specific teeth. An OPG shows all teeth and jaws in a single flat image; used for full-arch assessment and screening. A CBCT shows a three-dimensional volumetric dataset; used when three-dimensional anatomy is required for surgical planning. Each has a specific indication — they are not interchangeable, and the appropriate imaging is selected based on what clinical question needs to be answered.

















.webp)

.jpg)






